Chickenpox Symptoms Guide: Pediatrician Insights & Explanations
Article-at-a-Glance
Chickenpox typically begins with prodromal symptoms like fever and fatigue 1-2 days before the characteristic rash appears, giving parents a valuable early warning window
The chickenpox rash progresses through three distinct phases: papules (red bumps), vesicles (fluid-filled blisters), and crusts, typically lasting 5-10 days total
Chickenpox rash commonly starts on the trunk, face, or scalp before spreading to other body parts, with new spots continuing to form for several days
Unlike many other childhood rashes, chickenpox lesions appear in different stages of development simultaneously—a key diagnostic feature for parents and doctors
While most cases resolve without complications, parents should seek immediate medical attention for very high fever, signs of infected blisters, or respiratory distress
Chickenpox remains one of the most recognizable childhood illnesses despite widespread vaccination. Identifying the symptoms early helps parents prepare for the course of the disease and take appropriate measures to keep their child comfortable. Dr. James Pediatrics has been guiding parents through childhood illnesses for over 20 years, providing expert advice on recognizing and managing chickenpox symptoms in children of all ages.
While most children today receive the varicella vaccine, breakthrough cases and unvaccinated children still experience this highly contagious viral infection. Understanding what to expect, how to provide relief, and when to seek medical attention can make a significant difference in your child's comfort and recovery.

Early Warning Signs Before the Rash Appears
Chickenpox doesn't begin with the telltale rash. In the 24-48 hours before spots appear, children often display several prodromal symptoms that resemble a common cold or flu. Recognizing these early warning signs can help parents prepare for the course of illness and take preventive measures to avoid spreading the virus to others.
The incubation period for chickenpox ranges from 10-21 days after exposure to the varicella-zoster virus. During this time, the virus multiplies silently within the body without causing noticeable symptoms. Only in the final day or two before the rash erupts do the early warning signs become apparent.
Fever and Fatigue: First Indicators
A low to moderate fever, typically between 100-102°F (37.8-38.9°C), is often the first noticeable symptom of chickenpox. This fever may appear suddenly and be accompanied by pronounced fatigue and general malaise. Your normally energetic child might become unusually lethargic, wanting to rest more and participate less in regular activities. These symptoms often appear 24-48 hours before the first spots, providing an early warning window for attentive parents.
Headache and Decreased Appetite
Children with developing chickenpox frequently complain of headaches that range from mild to moderate in intensity. Appetite typically decreases significantly during this prodromal phase. Your child may show little interest in favorite foods or eat much smaller portions than usual.
These symptoms often coincide with general irritability and discomfort as the virus begins ramping up activity in the body. Younger children who cannot articulate their discomfort may simply appear fussy, clingy, or unusually difficult to console.
For many parents, these non-specific symptoms might not immediately suggest chickenpox until the characteristic rash appears. However, if you know your child has been exposed to chickenpox, these early symptoms should heighten your awareness of the potential for developing the illness.
Parent Insight: "My daughter's fever started on a Thursday evening, and I just thought it was a simple cold. She was unusually tired and barely touched her dinner. By Saturday morning, the first few spots appeared on her back and chest. Looking back, those early symptoms were our warning that chickenpox was coming." - Maria T., mother of 4-year-old
Mild Respiratory Symptoms
Some children develop mild respiratory symptoms during the prodromal phase of chickenpox. A slight cough, runny nose, or sore throat may be present, further mimicking the common cold and potentially delaying recognition of chickenpox as the underlying cause. These respiratory symptoms typically don't become severe and often resolve as the rash develops and the disease progresses into its characteristic phase.

The Classic Chickenpox Rash Timeline
The hallmark of chickenpox is its distinctive rash that evolves through several stages over approximately one week. Understanding this progression helps parents recognize the disease, track its development, and anticipate their child's needs throughout the illness. The chickenpox rash follows a predictable pattern while remaining highly individual in its severity and distribution.
What makes chickenpox unique compared to many other childhood rashes is that new spots continue to form for several days, meaning different areas of the rash will be in different stages simultaneously. This "crops" pattern of development—with some spots just appearing while others are already crusting over—is one of the most reliable diagnostic features of the disease.
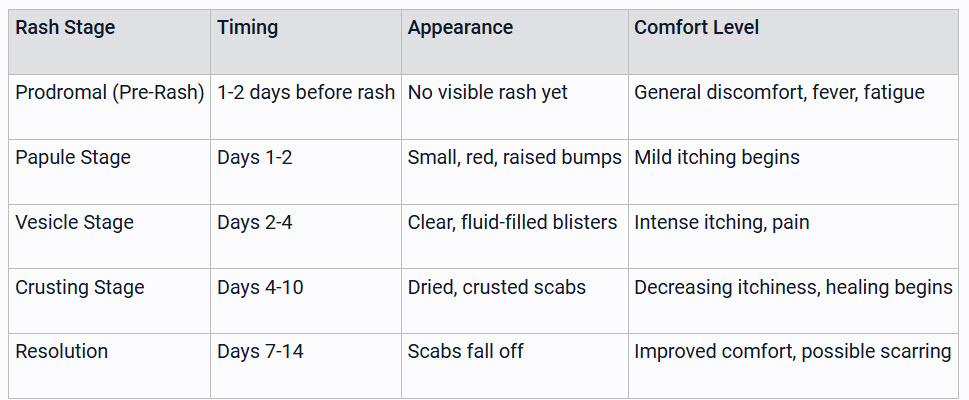
Day 1-2: Red Bumps (Papules) Emerge
The chickenpox rash begins as small, red bumps (papules) that often first appear on the chest, back, or face before spreading to the rest of the body. These initial spots may be mistaken for insect bites or heat rash as they're relatively few in number. Within hours, more papules develop, and the earlier ones begin transforming into the next stage. This initial eruption often coincides with the peak of fever as the body mounts its immune response against the virus.
Most children develop between 250-500 individual lesions during a typical case of chickenpox, though the number can vary greatly. Milder cases may have fewer than 50 spots, while severe cases can produce over 1,500 lesions covering most of the body surface. The density of the rash often correlates with the severity of systemic symptoms like fever and malaise.
Day 2-4: Fluid-Filled Blisters (Vesicles) Form
Within 24-48 hours, the red bumps transform into clear, fluid-filled blisters called vesicles. These small, tense blisters sit on a red base and contain viral particles in the clear fluid. This vesicular stage is when the chickenpox rash becomes most recognizable and most intensely itchy. The vesicles are typically 2-4mm in diameter and feel like small, firm bubbles when touched gently.
New crops of vesicles continue to form for 2-4 days, meaning your child will have lesions in different stages simultaneously. The vesicular fluid eventually becomes cloudier and more purulent before the blister ruptures or begins to dry out. This stage is when the illness is most contagious, and children should be kept isolated from others, especially pregnant women, newborns, and immunocompromised individuals.
Day 4-10: Crusting and Healing Phase
After 1-2 days as vesicles, the blisters break or dry out, forming golden-brown crusts or scabs. This crusting process starts centrally and works outward across the body as older lesions heal while newer ones are still forming. Once all lesions have crusted over, the child is no longer considered contagious, though this typically takes 5-7 days from the first appearance of the rash.
The crusts generally fall off naturally within 1-2 weeks, leaving either no mark or temporary red spots that fade over time. Deeper lesions, especially those that become infected or are repeatedly scratched, may leave permanent scars. Particularly severe cases can leave small, pitted scars similar to those seen with acne.

Where the Rash Typically Appears First
The distribution pattern of chickenpox follows a characteristic central-to-peripheral spread. The highest concentration of lesions typically appears on the trunk (chest, abdomen, and back), with moderate involvement of the face and scalp. Fewer lesions develop on the extremities, with the palms and soles usually being the least affected areas. This "centripetal" distribution—denser in the middle and less dense toward the extremities—helps differentiate chickenpox from some other childhood rashes.
The mucous membranes of the mouth, throat, eyes, and genital areas can also develop lesions, though they appear slightly different. Mucosal lesions rupture quickly to form shallow, painful ulcers rather than crusting over. These can make eating, drinking, or urination painful for children during the acute phase of illness.
How to Tell Chickenpox Apart From Other Rashes
Distinguishing chickenpox from other common childhood rashes is crucial for proper management and isolation when needed. Several features make chickenpox relatively distinct, though consultation with a healthcare provider is always recommended for definitive diagnosis. The hallmark characteristic that sets chickenpox apart is the presence of lesions in various stages of development simultaneously—fresh red bumps, fluid-filled vesicles, and crusting lesions all present at the same time.
Additionally, the distribution pattern of chickenpox is quite specific, with the highest concentration of lesions on the trunk and face, decreasing in density toward the extremities. This pattern, combined with the typical prodromal symptoms and the intense itchiness of the lesions, creates a clinical picture that experienced parents and healthcare providers can often recognize readily.
Key Differences Between Chickenpox and Hand-Foot-Mouth Disease

Chickenpox vs. Allergic Reactions
Clinical Pearl: "One reliable way to distinguish chickenpox from allergic rashes is by examining individual lesions. Chickenpox vesicles are typically uniform in size with a clear fluid center on a red base, while allergic hives are more variable in size, blanchable with pressure, and lack the characteristic fluid-filled center." - Dr. Sandra Miller, Pediatric Dermatologist
Allergic reactions often cause hives (urticaria) that can be confused with the early stages of chickenpox. However, hives typically appear and disappear rapidly, sometimes within hours, while chickenpox lesions persist and transform through their stages over days. Hives also tend to be larger, flatter, and more irregular in shape compared to the small, round, raised lesions of chickenpox.
Another distinguishing feature is that allergic rashes are rarely accompanied by fever before the rash appears, while chickenpox typically presents with prodromal fever. Allergic reactions also tend to respond to antihistamines with reduced itching and size, while chickenpox lesions show minimal response to these medications.
Heat rash (miliaria) might also be confused with early chickenpox, but heat rash typically appears in areas where sweat accumulates—skin folds, the neck, and areas covered by clothing. Heat rash also lacks the systemic symptoms like fever and malaise that accompany chickenpox.
If you're uncertain about whether your child has chickenpox or another type of rash, consult your pediatrician. Many offices can make arrangements to evaluate potentially contagious children without exposing other patients in the waiting room.

When to Call the Doctor Immediately
While chickenpox is typically a self-limiting illness that resolves without complications, certain symptoms warrant immediate medical attention. Recognizing these warning signs can help parents determine when home care is sufficient and when professional medical intervention becomes necessary. Most importantly, always trust your parental instincts—if something seems seriously wrong, don't hesitate to contact your healthcare provider.
When calling your doctor about suspected chickenpox, be sure to mention this concern before arriving at the office so appropriate isolation measures can be implemented. Many pediatric offices have specific protocols for evaluating potentially contagious patients to prevent exposure to other children in waiting areas.
High Fever That Won't Break
Seek immediate medical attention if your child develops a fever above 102°F (38.9°C) that doesn't respond to appropriate doses of fever-reducing medication, or any fever above 104°F (40°C). High, persistent fevers during chickenpox can indicate secondary bacterial infections or other complications requiring prompt intervention.
Contact your doctor if fever returns after initially improving, as this pattern often signals a secondary infection. This is especially important if the fever returns after several days of normal temperature, as it may indicate a complication rather than the primary viral illness.
Signs of Infected Blisters
While chickenpox blisters naturally contain clear fluid that may become slightly cloudy, signs of bacterial infection require medical attention. Watch for increased redness, warmth, swelling, or tenderness around blisters, particularly if the surrounding skin becomes increasingly red with red streaks extending outward. Pus-filled blisters that appear yellow or green, emit a foul odor, or are surrounded by expanding areas of redness may indicate a bacterial skin infection called impetigo.
Infected blisters can lead to more serious complications like cellulitis or, rarely, necrotizing fasciitis. These secondary bacterial infections may require antibiotics and, in severe cases, hospitalization for intravenous treatment.
Severe Symptoms Requiring Emergency Care
Difficulty breathing or rapid breathing
Severe persistent headache, especially with confusion or disorientation
Stiff neck with fever
Persistent vomiting or inability to keep liquids down
Severe abdominal pain
Unusual drowsiness or difficulty waking
Rapid heart rate at rest
Severe dizziness or balance problems
Unusual bleeding into the skin (beyond the typical rash)
These symptoms could indicate serious complications like pneumonia, encephalitis (brain inflammation), meningitis, or other severe secondary infections that can occur with chickenpox. Don't wait for a scheduled appointment if these symptoms develop—seek emergency care immediately.

Special Concerns for Infants Under 12 Months
Chickenpox in infants younger than 12 months requires special vigilance as they may be at higher risk for complications. Infants typically have less robust immune systems and limited maternal antibody protection, especially after 6 months of age. Call your pediatrician immediately if your infant develops chickenpox, particularly if they were premature or have any underlying medical conditions.
Warning signs in infants include poor feeding, decreased wet diapers, excessive sleepiness, inconsolable crying, or difficulty breathing. These symptoms may develop more rapidly in infants than in older children, so close monitoring is essential. Your pediatrician may want to evaluate an infant with chickenpox in person, regardless of symptom severity.
Warning Signs in Immunocompromised Children
Children with weakened immune systems due to conditions like cancer, HIV/AIDS, primary immunodeficiency disorders, or those taking immunosuppressive medications face significantly higher risks from chickenpox. For these children, even mild symptoms should prompt immediate medical evaluation. Varicella-zoster virus can spread more rapidly and cause more severe disease in immunocompromised patients.
In immunocompromised children, the infection can progress to organs beyond the skin, potentially affecting the lungs, liver, brain, and other vital organs. These children may benefit from early antiviral therapy and possibly varicella-zoster immune globulin (VZIG) to help limit the severity of infection.
Effective Home Treatments for Symptom Relief
While chickenpox must run its course, several home treatments can significantly improve your child's comfort during the illness. The primary goals of home care are managing fever, reducing itchiness, preventing skin infections from scratching, and maintaining hydration. With appropriate supportive care, most children recover completely from chickenpox within 1-2 weeks.
Safe Fever Management Options
Acetaminophen (Tylenol) can be safely used to reduce fever and discomfort associated with chickenpox. Follow the dosing guidelines for your child's weight and age precisely. It's crucial to avoid aspirin and aspirin-containing medications for children with chickenpox or suspected chickenpox, as these can increase the risk of a serious condition called Reye's syndrome.
Non-medication approaches to fever management include dressing your child in lightweight clothing, keeping room temperatures comfortable but not cold, and ensuring adequate fluid intake. Lukewarm (not cold) baths can help reduce fever and provide temporary relief from itching, but avoid vigorous rubbing when drying, as this can irritate the blisters.
5 Ways to Reduce Itching Without Scratching
Colloidal oatmeal baths: Add commercially prepared colloidal oatmeal to lukewarm bathwater to create a soothing solution that reduces inflammation and itching.
Calamine lotion: Apply this directly to itchy lesions to dry them out and relieve itching. Avoid calamine with antihistamines (diphenhydramine) as this can cause absorption issues.
Cool compresses: Apply cool, damp washcloths to particularly uncomfortable areas for 5-10 minutes several times daily.
Baking soda solutions: Mix 1 cup of baking soda in a tub of lukewarm water for a soothing bath alternative.
Oral antihistamines: Over-the-counter options like cetirizine or diphenhydramine can reduce itching from the inside out. Consult your pediatrician for proper dosing.
Keep your child's fingernails short and clean to minimize damage from scratching. For younger children, lightweight cotton gloves or socks pulled over the hands at night can prevent unconscious scratching during sleep. Distraction with games, books, movies, or other engaging activities can help take your child's mind off the discomfort.

Keeping Your Child Comfortable During Recovery
Maintaining good hydration is essential during chickenpox, especially when fever is present. Offer frequent small amounts of water, diluted juice, popsicles, or other appealing fluids. Children with mouth sores may prefer cool, non-acidic, and non-spicy foods and beverages that don't irritate the lesions. Smoothies, yogurt, mashed potatoes, and lukewarm soups can provide nutrition when appetite is poor.
Create a calm, cool environment with comfortable, loose-fitting cotton clothing that won't irritate the rash. Change bed linens frequently if they become soiled or damp. For severe cases, consider setting up a temporary "sick room" with activities, drinks, and comfort items to minimize movement when blisters are at their peak.
The Chickenpox Vaccine: Protection and Breakthrough Cases
The varicella (chickenpox) vaccine has dramatically reduced the incidence of chickenpox since its introduction in the United States in 1995. Before widespread vaccination, about 4 million cases occurred annually, resulting in approximately 10,000 hospitalizations and 100-150 deaths. Today, severe cases are much rarer, primarily occurring in unvaccinated individuals or as breakthrough infections.
Recommended Vaccination Schedule
The CDC recommends two doses of the varicella vaccine for children, adolescents, and adults who haven't had chickenpox. For children, the first dose is given at 12-15 months of age, and the second dose at 4-6 years (though it can be given earlier, provided at least 3 months have passed since the first dose). The two-dose regimen provides approximately 98% protection against any form of chickenpox and nearly 100% protection against severe disease.
Catch-up vaccination is recommended for older children and adults without evidence of immunity. For people 13 years and older who haven't had chickenpox or been vaccinated, two doses given 4-8 weeks apart are recommended. Certain high-risk groups, including healthcare workers, teachers, college students, military personnel, and international travelers, should ensure they're protected through either vaccination or confirmed previous infection.
What to Expect With Breakthrough Chickenpox
Breakthrough chickenpox refers to cases that occur in vaccinated individuals. These cases are typically much milder than natural chickenpox, with fewer lesions (usually less than 50), lower fever, shorter duration of illness, and faster recovery. The lesions in breakthrough cases may not progress through the typical stages—they might appear more like bug bites than the classic fluid-filled blisters and often don't form crusts. Despite being milder, breakthrough chickenpox remains contagious, though possibly less so than natural chickenpox.

How Long Is Chickenpox Contagious?
Chickenpox is highly contagious, with a transmission rate of 85-90% among susceptible household contacts. The virus spreads primarily through direct contact with fluid from blisters, respiratory droplets from coughing or sneezing, or airborne transmission. A person with chickenpox becomes contagious 1-2 days before the rash appears and remains contagious until all lesions have crusted over, typically 5-7 days after rash onset.
Preventing Spread Within Your Household
When one family member develops chickenpox, protecting others requires diligent preventive measures. Isolate the infected person as much as possible, especially from high-risk individuals like pregnant women, newborns, elderly family members, and those with compromised immune systems. Maintain separate sleeping arrangements if possible, and designate bathroom times with thorough cleaning between uses. Practice meticulous hand hygiene—frequent handwashing with soap and warm water for at least 20 seconds—and avoid sharing personal items like towels, washcloths, cups, or eating utensils.
When Your Child Can Safely Return to School
Children with chickenpox should remain home from school, daycare, and other public activities until all blisters have crusted over and no new lesions have appeared for 24 hours. This typically takes 5-7 days from the onset of the rash but may take longer in severe cases or in children with weakened immune systems. Most schools and daycare facilities have specific policies regarding return after infectious diseases—check your institution's guidelines for any additional requirements.
When your child does return to school, inform teachers and staff about their recent illness so they can be alert for signs of chickenpox in other children. If your child received antiviral treatment, they might be less contagious, but the same criteria for return (all lesions crusted over) still apply. Some mild residual crusts or red spots may remain visible for days or weeks but aren't contagious once fully dried and crusted.
Long-Term Immunity and Shingles Connection
After recovering from chickenpox, the varicella-zoster virus doesn't leave the body completely—it retreats into nerve tissue near the spinal cord and brain, where it remains dormant, often for decades. This infection typically provides lifelong immunity against future chickenpox infections. However, the dormant virus can reactivate years or decades later as herpes zoster, commonly known as shingles. This reactivation typically causes a painful, blistering rash along a specific nerve pathway. The risk of developing shingles increases with age and in situations of compromised immunity, such as during periods of significant stress, certain medications, or immune-suppressing conditions.

Frequently Asked Questions
Parents often have specific questions about chickenpox management, prevention, and long-term implications. These answers address common concerns based on current medical understanding and best practices for chickenpox care and prevention.
Can my child get chickenpox more than once?
It's extremely rare for a person to get chickenpox more than once. After a natural infection, most people develop lifelong immunity against the varicella-zoster virus. In the rare cases where second infections have been reported, they typically occur in people with weakened immune systems or may represent misdiagnosis of the initial or subsequent rash. What appears to be a second case of chickenpox is more commonly either a different viral rash or shingles, which is caused by reactivation of the dormant chickenpox virus rather than a new infection.
Should I expose my child to chickenpox on purpose?
Deliberately exposing unvaccinated children to chickenpox (sometimes called "chickenpox parties") is strongly discouraged by medical professionals. While chickenpox is typically mild in healthy children, complications can occur unpredictably even in otherwise healthy individuals. These complications can range from secondary bacterial skin infections to pneumonia, encephalitis, and even death in rare cases.
Vaccination provides immunity without the risks associated with the actual disease. The chickenpox vaccine has an excellent safety profile and protects not only the vaccinated individual but also helps protect vulnerable community members who cannot be vaccinated, such as newborns and immunocompromised individuals.
Can adults get chickenpox if they never had it as children?
Important Health Alert: Chickenpox in adults is typically more severe than in children. Adults have a 25 times higher risk of serious complications including pneumonia, encephalitis, and bacterial infections. Adults with no history of chickenpox should discuss vaccination with their healthcare provider, especially if they work with children or in healthcare settings.
Yes, adults who never had chickenpox as children can certainly contract the disease if exposed to the virus, and their cases tend to be more severe. The symptoms are similar to those in children but often more intense, with higher fever, more extensive rash, and greater risk of complications like pneumonia. Adults typically develop more lesions and have a longer recovery period compared to children.
Pregnant women who contract chickenpox are at particular risk. If infection occurs during the first 20 weeks of pregnancy, there's a small risk (about 2%) of congenital varicella syndrome, which can cause limb abnormalities, neurological problems, and other birth defects. Infection near delivery time can cause severe, potentially life-threatening infection in the newborn.
For these reasons, adults without immunity to chickenpox (either through previous infection or vaccination) should consider getting vaccinated, especially if they're in high-risk occupations like healthcare, childcare, or teaching.
What medications should be avoided during chickenpox?
Aspirin and aspirin-containing medications should be strictly avoided in children and teenagers with chickenpox due to the association with Reye's syndrome, a rare but serious condition that causes swelling in the liver and brain. Additionally, ibuprofen (Advil, Motrin) is sometimes avoided during chickenpox, though evidence for harm is less clear than with aspirin. Some medical professionals are concerned that ibuprofen might be associated with increased risk of certain bacterial skin infections, particularly group A streptococcal infections, in children with chickenpox. Acetaminophen (Tylenol) remains the preferred fever-reducer and pain reliever for chickenpox.
Does breastfeeding protect babies from chickenpox?
Breastfeeding provides some protection against chickenpox if the mother has immunity, but this protection is partial and temporary. Maternal antibodies against varicella-zoster virus can pass to the baby through breast milk, potentially reducing the severity of infection if the baby is exposed. However, this passive immunity is not complete and diminishes over the first few months of life.
If a breastfeeding mother develops chickenpox, she should continue breastfeeding if physically able. This provides the baby with antibodies that may help fight the infection. If the baby is under 3 months old or was born prematurely, consult a pediatrician immediately, as the doctor may recommend varicella-zoster immune globulin (VZIG) to provide additional protection.
The most reliable protection for infants comes from "cocooning"—ensuring that all household contacts and caregivers are immune to chickenpox through either prior infection or vaccination. This creates a protective buffer around vulnerable babies who are too young to be vaccinated.
For the most comprehensive and current information about chickenpox symptoms, prevention, and treatment, consult your child's pediatrician. Early recognition and appropriate management of symptoms can help ensure your child recovers comfortably and without complications from this common childhood illness.
